|
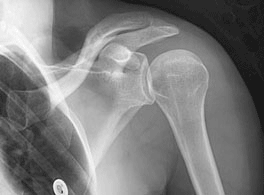
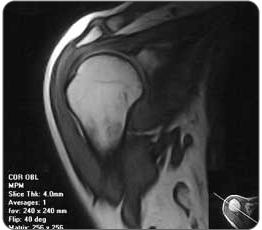
| Adhesive Capsulitis (Frozen Shoulder)Symptoms of Frozen Shoulder Frozen Shoulder is the catastrophe that often happens after a shoulder impingement injury is left untreated. True frozen shoulder requires a physician to diagnose, and there are three major signs* for diagnosing this condition:
You will often be unable to lift your arm over your head or away from your body nor will you be able to rotate it inwards; eventually you may not be able to move it at all. The lack of movement in your shoulder joint will interfere with your everyday tasks like getting dressed, driving, working; even completing simple things like reaching behind your back to scratch it. Muscle spasms in your rotator cuff muscles and swelling of your tendons will also limit your ability to move. Pain is generally experienced over the front and sides of your shoulder and upper arm area (around your deltoid, biceps brachii and rotator cuff muscles) which can radiate down to your elbow and wrist, or around your upper back from your trapezius muscle, because of the restricted joint space. You will experience pain with movement (such as trying to reach across your body) and eventually at rest. However depending on the cause of your adhesive capsulitis, it can be referred from other areas like your neck, heart, diaphragm, liver or spleen. 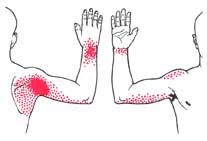 Weakness in your shoulder, upper arm and back muscles will occur over time from lack of use; this can create an imbalance in your muscle strength (as the stronger muscles have to compensate for the weaker ones) and cause muscular strains and alignment issues. Many people will experience depression, anxiety and psychological stress because of the secondary effects of the constant pain from adhesive capsulitis over the long term (stop working which leads to financial stress, stop participating in social and sports activities). Some people have even experienced an increase in body odor as they find it harder to reach and clean their armpit areas. Often there can be changes in your local nerves to your sweat glands. Causes of Frozen ShoulderThere is no definite cause for adhesive capsulitis, however it's believed to be a result of inflammation and scar tissue developing in your shoulder capsule which shrinks your capsule size and limits shoulder and humerus movement. It generally starts as a little pinch of pain around the long head of your biceps tendon that doesn't get better. The shoulder capsule then starts to stick to itself and wraps tightly around your joint. The inflammation spreads and causes swelling in your other tissues like your bursa. The amount of synovial fluid (which helps the shoulder joint move) is decreased causing pain and lack of movement in your shoulder joint. This condition can be a result of primary adhesive capsulitis or secondary adhesive capsulitis. Primary adhesive capsulitis occurs for no apparent reason (idiopathic cause). Secondary adhesive capsulitis is generally a result of changes in the structures and tissues supporting your shoulder and/or diseases.  There are a number of things that can cause damage to your shoulder muscles and tissues such as repetitive use or overuse from work or sporting activities, acute injuries and aging. Over the years your muscles will start to lose their mass and strength, your tissues will lose their elasticity and degenerate, making you more susceptible to injury. Weakened muscles and/or tendons or injuries to your rotator cuff (tears, impingements), arm or shoulder fractures, arthritis, bursitis, tendinitis or surgery can instigate adhesive capsulitis. You are at increased risk of suffering from this condition if your shoulder or arm have been immobilized or splinted and you haven't moved the area in a while. Adhesive capsulitis has also been linked to poor posture or slouching which shortens the ligaments around your shoulder joint. Some medical professionals believe adhesive capsulitis is caused from an autoimmune reaction, where your body's defense system attacks itself (it thinks its going after foreign material). This action causes inflammation in the tissues being attacked; as a result your shoulder freezes up.  Hormonal and genetic conditions also can influence your chance of experiencing adhesive capsulitis. People who suffer from diabetes, cardiovascular disease, heart disease, lung disease, chronic bronchitis, hyperthyroidism, hypothyroidism, Parkinson's disease, Dupuytren's contracture, or those who undergo breast surgery, heart attack or stroke (who are paralyzed on one side) where they are unable to move their shoulders through full range of motion for a period of time are at a higher risk as well. Adhesive capsulitis is 5 times more common in people with diabetes, affecting 10 - 20% of people who have it. Glucose molecules attach to collagen (connective and/or scar tissue) in people with diabetes, which builds up in the joint and can cause the shoulder to stiffen. Generally adhesive capsulitis occurs in people between 40 - 70 years of age; it is very rare in young people. 60% of women over 40 years of age have a risk of suffering from adhesive capsulitis, possibly as a result of hormonal changes during menopause. However it can occur in both men and women. Phases of Frozen ShoulderThere are three distinct phases of frozen shoulder that can all be identified by their symptoms: Stage 1: The freezing or painful phase During this stage you develop pain and stiffness in the shoulder joint. As the pain increases, movement becomes more difficult and the shoulder is used less. Often your back and neck muscles start to ache as they work harder to compensate for fewer shoulder movements. This stage can last from a few weeks to a few months. Stage 2: The frozen or stiffening phaseIn the next stage, you will notice that the stiffness remains but the pain does not become worse and may even start to decline. This stage usually lasts anywhere from 4 months to nearly a year. Stage 3: The thawing phaseFinally, you will find that the full range of movement begins to return to the shoulder joint. This stage usually takes a minimum of 5 more months but may take as long as 2 years. Who's at Risk?Below are general factors and conditions are common among people who suffer from frozen shoulder:
The more specific risk factors are as follows: Specific Risk Factors for Developing Frozen ShoulderIf you exhibit any of these Frozen Shoulder risk factors, then you need to increase your awareness of the condition and more importantly, take early steps to help prevent the condition from developing. Diabetes:Approximately 20% of diabetics will develop one or more Frozen Shoulders during their lifetime. This compares to only 2% of the non-diabetic general population according to the American Academy of Orthopedic surgeons. A ten times greater risk factor is truly significant. While researchers are still trying to determine exactly why diabetics are prone to Frozen Shoulder, there are some theories with scientific backing that help to make the determination. One theory involves the metabolism of glucose and its affect on collagen. First of all, collagen is one of the main building blocks of soft tissue such as ligaments and tendons. The ligaments stabilize the joint by holding the bones in place while tendons connect the muscles to the bone, allowing for proper muscle function and also greater stability of the joint. As we know, diabetics are unable to properly metabolize glucose. A simple sugar that provides fuel for all cells in the body, glucose is critical for numerous metabolic functions. In diabetics, it has been shown that glucose will attach itself to collagen tissue, in particular within the shoulder. While not fully understood why the shoulder is targeted, it does happen and the abnormal build-up of glucose on the collagen causes the shoulder to stiffen. In a healthy body, collagen fibers normally move in concert with one another during movement of the muscle. In the case of diabetics, glucose binds the collagen fibers together (almost like a glue substance) and this limits the extensibility of the fiber. This phenomenon is known as Glycosylation. The immobilization of the collagen fibers causes the shoulder to freeze and limit functional ability of the shoulder overall. Age & GenderFrozen Shoulder predominantly affects middle aged women between the ages of 40 and 60. Trauma to Shoulder or ArmIndividuals who sustain a traumatic shoulder injury or undergo shoulder surgery are at risk for developing frozen shoulder. Following these scenarios, the shoulder joint will be immobilized for a number of weeks. During this time, the body naturally makes an attempt to begin healing itself by producing a weak form of collagen (scar tissue) to help fuse the torn/cut tissue and to lay in place the foundation to heal. Problems arise when the injured tissue (through immobilization) fails to receive the enhanced blood flow it needs to properly regenerate new, healthy tissue. As a result, the scar tissue continues to build to unprecedented levels. Eventually, the accumulation of scar tissue will bond to healthy tissue within the joint capsule - and such bonds further restrict movement of the shoulder. AutoImmune Disorders & Thyroid IssuesHyperthyroid patients and those dealing with autoimmune disorders produce excess amounts of cytokines (chemical messengers) along with excess fibrous connective tissue - two factors that could lead to the development of Frozen Shoulder. Cytokines play a pivotal role in the generation and management of immune and inflammatory responses. When produced in excess amounts, the body (and specifically, the immune system) are thrown into chaos. What results is an abnormal immune response of the body against cells and tissues found throughout the body, including the shoulder. In essence, the immune system can not differentiate between normal and abnormal substances and sets itself on a course of self-destruction. Over time, the shoulder joint capsule can slowly weaken and break down, leading to stiffness and general weakness of the shoulder. What is interesting is that one portion of the immune system is attacking the body while other segments of the immune system will attempt to heal the damage that is being done. The end result is an excess build-up of fibrous tissue that once again - bonds to healthy tissue and causes loss in range of motion - the Frozen Shoulder so to speak. In addition, hyperthyroid suffers produce an excess amount of Thyroxin - a hormone critical in the metabolic function of the body. When excess amounts of Thyroxine is produced, the body is unable to properly metabolize it and an autoimmune response ensues (inflammation and breakdown of healthy tissue). On the other end of the spectrum, there is a segment of Frozen Shoulder sufferers who are hypothyroid - meaning their bodies do not produce enough of the thyroid hormone - Thyroxine. Hypothyroidism results from the thyroid gland being unable to make enough thyroxine, which causes many of the body's functions to slow down. Included is the ability of the body to remodel damaged muscle and connective tissue. The body lacks the fuel it needs to heal - resulting in a long recovery process, especially in the case of Frozen Shoulder. You need to strongly recognize that if left untreated or improperly treated, frozen shoulder will typically last about 24 months. You will suffer through three distinct phases (sometimes called "3 stages of frozen shoulder"). If certain simple measures are taken, recovery can be accelerated. * Nearly all patients recover from frozen shoulder, but many often recover with a permanently reduced Range of Motion (ROM). * Dias R, Cutts S, Massoud S. Frozen shoulder. BMJ?: British Medical Journal. 2005;331(7530):1453-1456. Diagnosing Frozen ShoulderThere are several range of motion movements that can help diagnose adhesive capsulitis. Your doctor may ask you to:
If there is limited range of motion for one or more of these movements, your doctor will probably recommend further diagnostic testing.  To help your doctor or orthopedic surgeon achieve a proper diagnosis, he/she will begin with a medical history about you, your current condition and symptoms. He/she will inquire about the intensity of your present pain, the duration of your symptoms and the limitations you are experiencing. Details about what instigated the problem, when it started, and whether or not you have ever had treatments for this or a similar condition in the past, are very helpful in assessing your injury. A physical examination will be performed to determine if you have any signs of adhesive capsulitis or other shoulder injury. Your doctor will visually assess and press on the bones and soft tissue in both your shoulders to evaluate sameness (symmetry) and recognize differences. This will identify any abnormalities, such as mild or severe inflammation, tenderness, fluid, bone or tissue deformity, weakened muscles, redness and/or warmth on the skin. He/she may ask you to complete a series of arm movements, such as raising your arms to the front, back and side, to measure your range of motion and see what causes pain and tightness. Some of these will be performed by you and others will be performed by the doctor. Generally you will not be able to move your arm in any direction at all (or just slightly) if you have adhesive capsulitis - whether you try to move it or your doctor tries to move it. If you have movement when your doctor moves your arm, you may be tested for other shoulder conditions. Most Common Shoulder Diagnostic Tests: Diagnostic tests will often help to obtain more detailed information about your shoulder condition.
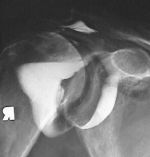 Arthrogram contrasts are special x-rays that show details of the shoulder capsule, such as a decrease in size (in a normal shoulder the capsule is rounded, but in a frozen shoulder the capsule is squat, square and contracted). Blood testing can be done if the doctor suspects the primary reason for your frozen shoulder is a result of a systemic disorder Steps for Treating Frozen ShoulderStep 1: Reduce Pain & InflammationInflammation is the body's natural response to a ligament, tendon, muscle (or ANY soft tissue) injury and is a normal part of the healing process - helping to reduce tissue infection in the early stages of injury. Swelling, pain, heat sensation, redness, and loss of function are the main symptoms experienced. The combination of cold therapy and static compression is the gold standard in medicine for minimizing tissue damage and reducing inflammation in the acute stage of injury or activity. It serves as a critical bridge into next phase of the healing process. Step 2: Enhance Blood Flow to the Shoulder Joint CapsuleLigaments and tendons are considered dense soft tissue. As a result, they naturally receive quite limited blood flow and this is precisely why injuries to these tissues take so long to heal. The challenge is, how do you effectively increase blood flow to soft tissue?
 An injury that often leads to straining in other areas will make an overall recovery hard to initiate. People tend to "chase the pain", meaning they only focus on treating an area that is actively painful, while not taking into account the fact they other areas of the body will be overcompensating...eventually leading to issues in those areas as well. Heat energy generated by the TShellz Wraps® operate by increasing blood flow in tissue in an near the area of application. The objective of the TShellz Wrap® is to increase blood flow in these targeted areas, resulting in relaxation of the vessel walls. The vessels then gently expand, allowing for more nutrient rich blood to reach the damaged tissues. Plus, the enhanced blood flow helps in flushing waste and fluid build-up from the injury site - further enhancing the ability of the body to heal. With a TShellz Wrap® application, more blood now begins to flow effectively to tissue within the treatment area - for the length of the treatment and a short duration thereafter. Soft tissue needs substantial blood flow to heal as it is through the blood the body carries the oxygen and nutrients needed for proper and long-term healing. With dedication, the right tools, and the right information - you will achieve your goal of a sustainable recovery while minimizing scar tissue growth and maximizing your range of motion. When it comes to frozen shoulder, our goal is to do everything we can to get rid of your condition as soon as possible while winding up with no loss of Range of Motion (ROM); remember that permanent loss of ROM is a common issue with frozen shoulder sufferers even after their frozen shoulder has completely healed. A combination approach of cold compression, TShellz Wrap®, stretches and proper support will give you the best chance of recovering fast, fully and without ROM loss. True, effective healing will differ from person to person, but we have witnessed that best results come from those that take a comprehensive, dedicated approach.  If you have questions, call our office at 1-866-237-9608 (toll free continental US). Surgical Treatments for Adhesive Capsulitis/Frozen ShoulderManipulation Under Anesthesia (MUA)Manipulation is an aggressive approach that involves stretching the shoulder while you're under general anaesthetia. You get put to sleep during this procedure as the process of forcing your shoulder through the full range of motion (past your point of comfort) can be quite painful. This procedure is basically meant to tear and rip up the scar tissue in your joint to force a new healing cycle for new swelling, inflammation and tissue repair. The hope is that this procedure will get the range of motion back in your shoulder.  In order to make sure your frozen shoulder injury doesn't come back, you'll have to go to physical therapy afterwards to maintain shoulder mobility. You probably won't notice an immediate difference or change in your range of motion. Many patients have to wait a few weeks to regain their range of motion after this procedure - a recovery process that requires physical therapy and conservative treatment methods. (reference: 1) The doctor will probably suggest this procedure when you're in the 'frozen' stage of your injury. Usually it's done at a time when your pain has decresed but you've reached the point where you have the most limtied range of motion since your injury started. This type of procedure is usually done for those suffering from frozen shoulder without any other injury or condition - that includes other shoulder soft tissue injuries (ie. rotator cuff tear, impingement syndrome) or diabetes. Those who are diabetics usually end up having their shoulder refreeze on them 2 to 3 weeks after a manipulation procedure. (reference: 1) 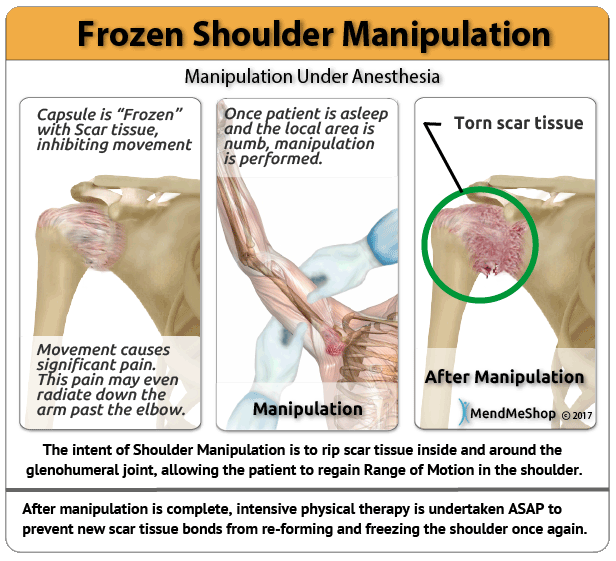 After the procedure is done you may be injected with a local anesthetic to help you deal with the pain. Sometimes this process is also combined with a steroid injection into the shoulder and once completed. Manipulation can be very effective but in many cases it can create more injuries and make your shoulder even worse. Other injuries - like bone fractures, dislocation of the shoulder joint, rotator cuff tears and complications such as stretching and possibly tearing of the soft tissues in your shoulder (rotator cuff muscles and tendons, ligaments, cartilage, joint capsule), increasing inflammation and scarring in the shoulder joint, dislocating or fracturing your arm bone, neurovascular injury to your brachial plexus or other nerves, and severe osteopenia (reduction in bone mass or density) - have been known to happen from manipulation. This procedure requires aggressive rehabilitation. Arthroscopic or Open Capsular Release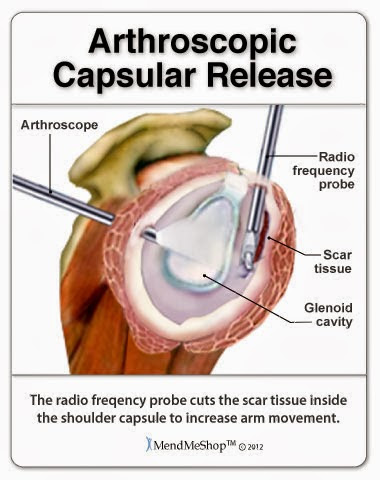 The lining of the shoulder joint is know as a "capsule". This capsule is normally very elastic and flexible, allowing the shoulder to maintain a large range of motion. In the case of frozen shoulder, this capsule loses its elasticity through inflammation or damage / tearing to the surrounding ligaments. When this happens you lose range of motion and experience a great deal of pain in the area. Occasionally an arthroscopic exam or open surgical procedure is required to release a tight shoulder joint capsule, especially when you have a very adhesive capsulitis after an injury, trauma or fracture (often used with diabetics as well). Arthroscopic surgery involves making tiny incisions around your shoulder joint and inserting a pencil-thin, fiber optic camera with a small lens and lighting system in one hole, and small surgical instruments in the other holes. The surgeon will take a look inside your joint to investigate all the soft tissues and bones. These images will then be transmitted to a TV monitor, which allow the doctor to make a diagnosis and/or perform the adhesive capsulitis surgery under video control. At the end of surgery, your incisions are closed, and a dressing is applied. 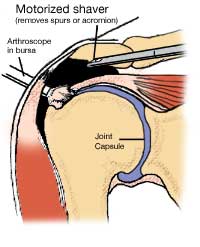 Arthroscopic capsular release involves cutting the tight portions of your joint capsule, scar tissue and your coracohumeral ligament. This frees your joint which alleviates pain and returns your full range of motion. Results are seen faster with this surgery than with MUA, and this surgery can be repeated a few times if inflammation and scar tissue persist. However, if shoulder movement isn't regained, open surgery may be required (a larger incision is made to have better access to the shoulder). Complications with this surgery involve persistent stiffness and pain. An arthroscopic or open capsular release surgery will remove scar tissue within the shoulder capsule. Once this tissue is removed, the capsule will hopefully be more flexible allowing you to regain mobility in the shoulder joint. The success rate for capsular release surgery is over 95%, though in some cases, more surgical intervention may be required for scar tissue removal, especially if you have undergone open surgery vs arthroscopic. 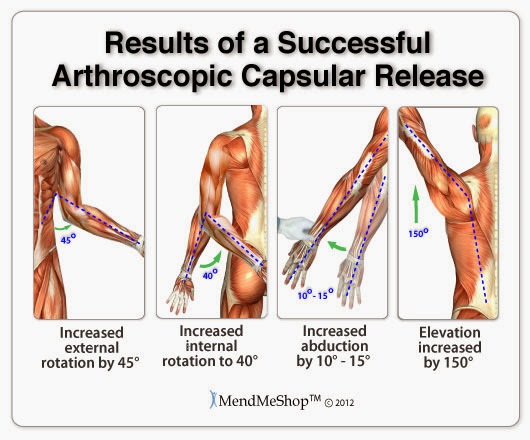 The capsular release surgical technique can be completed through Arthroscopic surgery, Open surgery or a combination of both procedures. With most frozen shoulder injuries, arthroscopic surgery is the preferred procedure because it's minimally invasive and patients usually recover at a much faster rate. This type of surgery will provide the surgeon with first hand insight into the nature of the injury and possibly limit the amount of shoulder damage from surgery - helping to promote a more effective recovery. Some cases however, will require open surgery as the scope of arthroscopic surgery is limited in comparison to full exposure of the shoulder capsule in open surgery. If you undergo an open surgery for your frozen shoulder, you should expect a longer time for rehabilitation efforts. The Path to RehabilitationIf you've had surgery on your shoulder or other soft tissue in the area, then your doctor will quickly get you on the path to rehabilitation. The aggressiveness of your rehabilitation efforts and your injury's ability to heal will depend on a variety of factors including (but not limited to):
Know that no 2 rehabilitation plans are alike - The less invasive your surgery is, the quicker your road to recovery will be. The goal of a rehabilitation plan is to manage pain and swelling while improving function, strength, and range of motion. Ultimately, you'll regain enough strength in your shoulder to be able to move it around and return to activity. 
You'll most likely spend a lot of time with a physical therapist after your surgery, but as your healing progresses emphasis will be placed on your personal at-home treatment.
The success of your rehabilitation will depend on your dedication to working with your doctor and physical therapist while also managing your recovery on a daily basis at home. No matter what type of surgery you've had (or even if you don't need surgery at all), your home therapy routine can be improved by controlling initial and on-going pain/swelling, increasing blood flow in the localized shoulder area, and incorporating daily stretches to increase range of motion so that you can achieve long-term, positive results.  All of this can easily be done by incorporating the use of a Cold Compress or Ice Pack and a Shoulder TShellz Wrap® into your conservative treatment home rehabilitation routine. Proper and regular usage of these tools will decrease your time spent in recovery and reduce the risk of re-injury. Post-Surgery Shoulder StabilityDuring the first 24 to 72 hours after the surgery your shoulder will be tender, swollen and very painful. Your shoulder may be weak and unstable, and depending on your procedure, you may have to wear an arm sling for at least 1 week. The most important aspect of frozen shoulder surgery is the rehabilitation afterwards, because those who don't stretch and use conservative treatment methods usually have their frozen shoulder injury come back within a few weeks. There is always a possibility of re-injuring your shoulder even after a surgical procedure has been done. Ask any doctor and they'll tell you that the success of your surgery depends on your level of dedication to regular at home care of your shoulder. Most of our frozen shoulder post-op clients have treated themselves successfully through regular use of the Shoulder TShellz Wrap. Using these therapies will lessen the chance and/or severity of shoulder joint degeneration and surrounding muscular atrophy during your rehabilitation process. In some cases our customers have prevented the onset of degeneration through regular use of these treatments. They will even combine these therapeutic treatments with the rehabilitation plan recommended by their doctor, surgeon or physical therapist. Our Shoulder Treatment Formula is Proven to Work!We are very confident our TShellz Wraps and accessory products will assist you in recovering from your injury by reducing your swelling and inflammation induced pain, maximizing blood flow where it's needed most and increasing the flexibility / range of motion of your shoulder with consistent, safe stretching.  Here at AidMyRotatorCuff we pride ourselves in helping you with your healing and recovery process. Everyone at AidMyRotatorCuff has tested and used the products, finding solutions to conditions that do not fit into the norm. This dedication to our customers and our products goes hand-in-hand with our guarantees to you as a customer:
 
Click HERE to Go To Our Online Store We take all major credit cards and Paypal. If you are on your mobile phone, Click to Call Our Office (toll free continental NA). Our customer service lines are open 5 days a week helping people understand their injuries and how to treat them. Simply call toll free 1-866-237-9608 to talk with one of our knowledgeable Product Advisors. They have the ability to answer questions and even put together a treatment plan for you. Yes, they are that good. See for yourself.The TShellz Wraps® are FDA Registered Medical Devices, are suitable and completely safe for patients to use themselves at home (as instructed). The TShellz Wrap® is a high quality device. This neoprene shell helps shape the flexible Energy Pad to mold around the contours of the joint, ensuring there is an even distribution of energy within the coverage area. Once treatment is complete, you also have the option of tightening the straps to provide light compression support for your injured joint. You can also unplug the device from the power supply enabling you to move around the home, office or clinic freely and still use the wrap for support and comfort. The TShellz Wrap® is an effective treatment tool intended to help maximize the body's own healing process. As a side benefit, you will also find it to be very comfortable to wear at any time. Click HERE to Go To Our Online Store We take all major credit cards and Paypal. Product specialists are available 9:00 am to 5:00 pm Eastern Standard Time Monday to Friday. If any question or concern arises, call us or simply send us an email at any time (we check our emails constantly all throughout the day and night.. even on holidays!). We will respond as soon as possible. North America Toll Free 1-866-237-9608 |
|